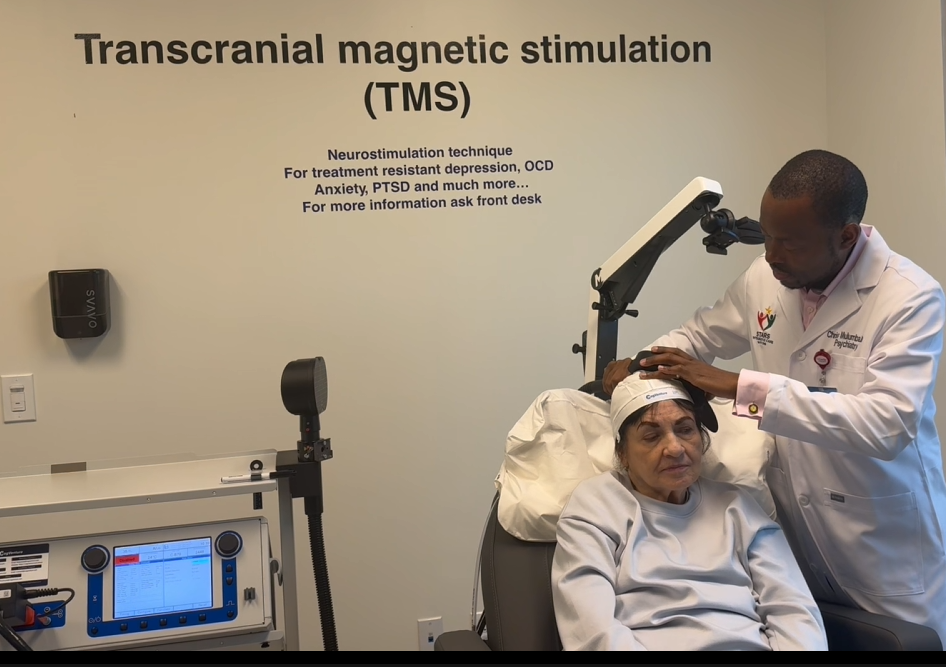
How TMS Therapy Works: The Neuroscience Behind the Treatment (Part 2)
By Dr. Chriss Mulumba, MD | Board-Certified Psychiatrist | STARS Integrative Care, Suwanee, GA
If you read Part 1 of this series, you know the basics: TMS is FDA-cleared, non-invasive, medication-free, and works for people who haven’t gotten adequate relief from antidepressants. But I find that many of my patients — and many people who are just starting to research TMS — want to go deeper.
They want to know: what is actually happening in the brain during a TMS session? Why does stimulating one area of the brain improve depression? What are the different types of TMS, and does the type matter?
Those are exactly the right questions. Understanding the science behind TMS doesn’t just satisfy curiosity — it helps you become a better advocate for your own care. So in Part 2, let’s go deeper.
The Depressed Brain: What’s Actually Happening
Depression is not simply a chemical imbalance. That’s a simplified version of a much more complex story. What we actually see in people experiencing major depression is a pattern of dysregulation across specific brain networks — areas that govern mood, motivation, attention, and emotional processing.
One of the most consistently identified findings in brain imaging studies of people with depression is reduced activity in the left dorsolateral prefrontal cortex (dlPFC). This is the region located at the front and sides of your brain, just behind your forehead. It plays a critical role in regulating mood, decision-making, and emotional responses.
When this region is underactive, the brain’s ability to regulate negative emotions and sustain positive ones is compromised. This contributes to many of the hallmark symptoms of depression: persistent low mood, loss of interest, difficulty concentrating, and emotional heaviness that medications alone sometimes can’t fully lift.
TMS targets this region directly. Rather than trying to adjust brain chemistry through a medication taken systemically (affecting the entire body), TMS delivers focused magnetic pulses precisely to the dlPFC — with the goal of reactivating and normalizing its function over time.
Why the Left dlPFC? |
|
Research consistently shows it is underactive in major depression |
|
It regulates mood, executive function, and emotional control |
|
It is anatomically accessible from the scalp surface |
|
Stimulating it produces measurable changes in connected brain networks |
|
This is the target validated in FDA-cleared TMS protocols for MDD |
How Magnetic Pulses Change the Brain
Here’s the part that surprises most people: a TMS coil is placed against the scalp and generates a magnetic field that passes painlessly through the skull and induces a small electrical current in the underlying brain tissue. This current causes nearby neurons to fire.
Think of it like a gentle, precise wake-up call to neurons that have gone quiet.
When neurons fire repeatedly in a coordinated pattern over many sessions, something important happens: the connections between those neurons and the wider brain network begin to strengthen. This is neuroplasticity — the brain’s ability to rewire itself in response to repeated stimulation.
TMS isn’t a one-time fix. It’s a process. Each session builds on the last. Over a standard course of 36 sessions across six to nine weeks, the cumulative effect is a measurable shift in how the dlPFC and its connected regions function. For many patients, this translates into lifting of depression symptoms that medications couldn’t fully address.
The Different Types of TMS: What You Should Know
Not all TMS is the same. Over the years, the field has developed several distinct protocols. Here is a clear breakdown of what each one is, and how they compare.
- Repetitive TMS (rTMS) — The Standard Protocol
This is the original FDA-cleared form of TMS for major depressive disorder. It delivers repeated magnetic pulses in a steady rhythm to the left dlPFC — typically at 10 Hz (10 pulses per second). Sessions last approximately 20-37 minutes. A full course is 36 sessions over about 6-9 weeks, scheduled five days per week.
rTMS has the most extensive clinical evidence behind it and is the protocol used at STARS. It is covered by major private insurance carriers for qualifying patients with treatment-resistant depression.
- Deep TMS (dTMS) — Deeper Reach
Deep TMS uses a specialized H-coil design that allows magnetic pulses to penetrate deeper and across a wider area of brain tissue than standard rTMS. The FDA has cleared dTMS for both depression and obsessive-compulsive disorder (OCD).
It is particularly noted for its potential effectiveness in patients who have not responded to standard rTMS, though access and insurance coverage vary.
- Theta Burst Stimulation (TBS) — Accelerated Treatment
Theta burst stimulation is a newer, FDA-cleared protocol that delivers pulses in short bursts mimicking the brain’s natural theta rhythm. The major advantage: a full TBS session takes only 3-6 minutes, compared to 20-37 minutes for standard rTMS.
Intermittent TBS (iTBS) is applied to the left dlPFC to stimulate it, just as in standard rTMS — but in a fraction of the time. Evidence supports its effectiveness as comparable to standard rTMS for many patients. At STARS, we stay current on protocol developments to ensure patients have access to the most appropriate options.
| Protocol | Key Characteristics |
| Standard rTMS | 10 Hz, 20-37 min/session, 36 sessions — most studied, covered by major insurance |
| Deep TMS (dTMS) | H-coil, deeper reach, FDA-cleared for depression + OCD |
| Theta Burst (TBS/iTBS) | 3-6 min/session, mimics natural brain rhythm, FDA-cleared, growing evidence base |
What Happens in the Brain Over Time
The changes from TMS don’t happen all at once. Here is a general picture of the progression that research supports — though individual experiences vary:
| Treatment Phase | What’s Happening in the Brain |
| Sessions 1–5 | Neurons in the dlPFC begin responding to stimulation; no major symptom changes yet |
| Sessions 6–15 | Neural activity patterns start to shift; some patients begin noticing subtle mood changes |
| Sessions 16–25 | Network connectivity strengthens; many patients report meaningful symptom improvement |
| Sessions 26–36 | Consolidation of neuroplastic changes; full therapeutic effect often realized |
| Post-treatment | Effects can persist for a year or longer; maintenance sessions may extend benefit |
I always tell my patients at STARS: the early sessions are not wasted even if you don’t feel anything yet. You are building something. The brain changes incrementally, and most patients begin to notice a shift somewhere between weeks 3 and 5 of treatment.
Is TMS Safe? What the Evidence Shows
TMS has a well-established safety profile built from decades of clinical research and hundreds of thousands of patients treated worldwide. It is non-invasive, does not require anesthesia, and does not affect memory or cognition — a significant advantage over electroconvulsive therapy (ECT).
The most common side effect is mild scalp discomfort or a headache during or after the first few sessions, which typically resolves as patients adjust to treatment. Serious side effects are rare.
TMS is not appropriate for everyone. Patients with metallic implants in or near the head, certain types of pacemakers, or a history of seizures may not be eligible. Every patient at STARS undergoes a thorough evaluation before treatment to confirm candidacy.
TMS Safety Snapshot |
|
FDA-cleared since 2008 for major depressive disorder |
|
Non-invasive: no surgery, no sedation, no anesthesia |
|
No memory or cognitive side effects |
|
Most common side effect: mild scalp discomfort (usually temporary) |
|
Serious adverse events are rare in properly screened patients |
|
Not appropriate for patients with certain metallic implants near the head |
What This Means for You
Understanding the neuroscience of TMS matters because it reframes the question. This isn’t a last resort. This isn’t experimental. This is a targeted, evidence-based intervention that works with the brain’s own capacity for change.
If you or someone you love has been living with depression that hasn’t fully responded to medication, TMS may be a meaningful next step. At STARS Integrative Care, we verify your insurance before your first visit so you know exactly what to expect — financially and clinically.
In Part 3, we’ll walk through exactly who is a good candidate for TMS, how to prepare for your first session, and what the journey looks like from initial consultation to completion.
|
Ready to Learn If TMS Is Right for You? |
|
Call us: (470) 253-1350 |
|
Visit: starsmedpsych.com |
|
Location: 4330 Johns Creek Pkwy, Suite 400, Suwanee, GA 30024 |
|
Insurance accepted: Aetna, Blue Cross Blue Shield, Cigna, United Healthcare, Humana |
|
We verify your benefits before your first appointment. |